1 Roosevelt Avenue, Suite 203 Peabody, MA 01960
Dental Implants and Diabetes: A Guide for Peabody Patients

Diabetes affects over 38 million Americans, according to the CDC, and millions of those same people are also dealing with tooth loss. So it makes sense that one of the most common questions Dr. Brzoza hears at Coastal Dental Arts is some version of this: “Can I actually get implants with diabetes?”
The short answer is: often, yes. But the longer answer is what most people actually need to hear, because diabetes does change the picture – not necessarily in the direction patients assume.
This guide is written for patients considering dental implants who also happen to be managing diabetes. It’s grounded in current research, honest about the risks, and focused on what you can actually do to improve your outcome.
Why Diabetes and Dental Health Are More Connected Than You’d Think
The relationship between diabetes and oral health runs deeper than most people realize. Uncontrolled blood sugar creates a ripple effect in the body that directly impacts the mouth – specifically the gums, bone tissue, and the body’s ability to fight infection.
Research consistently shows that people with poorly managed diabetes are more prone to periodontal (gum) disease, slower wound healing, and a higher risk of oral infections. In fact, a 2022 systematic review published in Diabetes Care confirmed a bidirectional relationship between periodontitis and diabetes: each condition can worsen the other if left unaddressed.
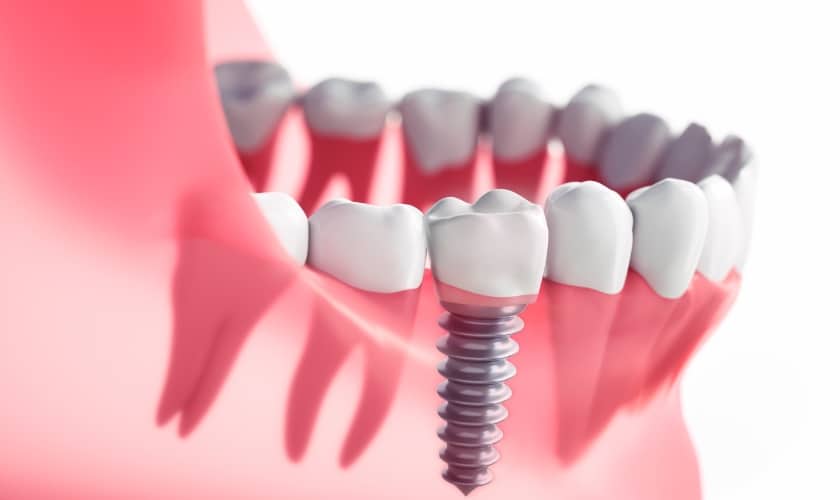
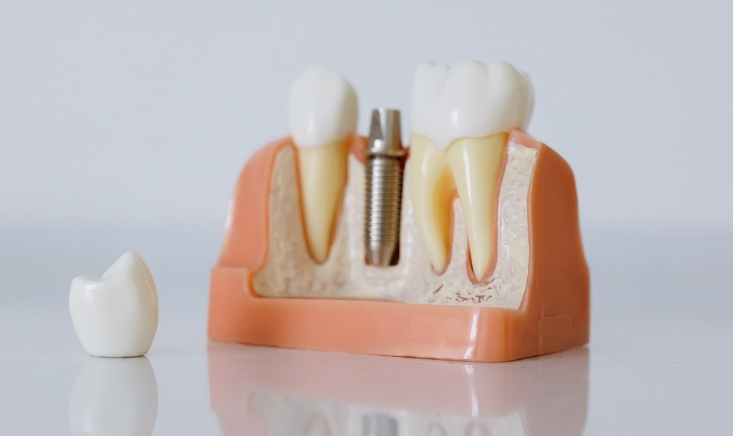
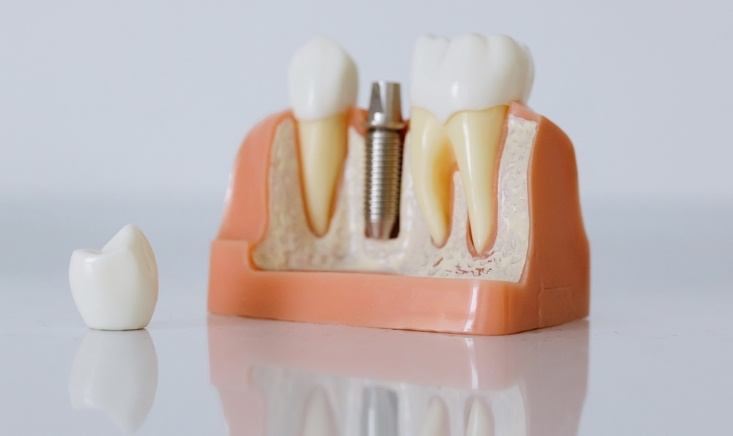
For someone considering dental implants, this matters a lot. Implants depend on osseointegration – the process where the titanium post fuses with your jawbone. Anything that disrupts healing or circulation can compromise that process. That’s where diabetes enters the conversation.
Does Diabetes Disqualify You From Getting Implants?
Not automatically, no. The key variable is blood sugar control. Patients whose diabetes is well-managed — particularly those with a stable HbA1c level (a measure of average blood sugar over the past two to three months) — tend to have implant success rates comparable to those of non-diabetic patients.
A landmark study published in the Journal of Dental Research found that patients with controlled type 2 diabetes had implant survival rates above 95% over five years, closely matching those of the general population. The difference emerged in patients with poorly controlled diabetes, where complication rates rose significantly.
The takeaway: your HbA1c number matters more than your diagnosis. Before recommending implant surgery, Dr. Brzoza will review your recent medical history and, in many cases, coordinate with your primary care provider or endocrinologist to confirm your blood sugar is in a range that supports safe healing.
Specific Risks Diabetic Patients Should Know About
Being informed isn’t the same as being scared off. These are real considerations that your care team will actively plan around:
- Slower healing: Elevated blood glucose impairs the body’s repair mechanisms, which means post-surgical recovery can take longer. Your provider will space out treatment phases accordingly.
- Increased infection risk: Bacteria thrive in high-sugar environments. Patients with diabetes have a higher baseline susceptibility to oral infections, including peri-implantitis — inflammation around the implant that can threaten its stability.
- Reduced bone density: Long-term diabetes, particularly when poorly controlled, is associated with reduced bone mineral density. Adequate jawbone volume is essential for implant placement.
- Medication interactions: Some diabetes medications can affect bleeding time or healing. A full medication review before surgery is non-negotiable.
None of these factors is a dealbreaker on its own. They’re variables, and variables can be managed with the right preparation.
How to Improve Your Candidacy Before Your Consultation
There’s meaningful work you can do before your first appointment, and it pays off.
- Get your HbA1c tested: If it’s been more than three months, ask your provider for an updated reading. Ideally, you’d want to arrive at your consultation with an HbA1c below 7.0% – though some patients with levels up to 8.0% may still be good candidates depending on other health factors.
- Address any active gum disease first: Periodontal disease and implants don’t mix. Treating existing gum issues before implant placement is standard protocol, particularly for diabetic patients.
- Commit to a rigorous home care routine: Brushing twice daily, flossing, and using an antibacterial rinse decreases your risk of infection both before and after surgery.
- Loop in your medical team: Your dentist and your diabetes care provider should be on the same page. Coastal Dental Arts regularly collaborates with patients’ physicians when medically complex cases arise.
Life in Peabody With Implants: What the Recovery Looks Like
For most patients, diabetic or not, the implant process unfolds over several months. The titanium post is placed first and given time to integrate with the bone before the final crown is attached. For diabetic patients, this timeline may be extended slightly to allow for thorough healing between stages.
Coastal Dental Arts serves patients throughout the North Shore area, including Peabody, Salem, Danvers, and Lynnfield. Post-surgical follow-up is built into the process, not an afterthought. Dr. Brzoza monitors healing closely, particularly in the weeks immediately after placement when infection risk is highest.
Patients managing diabetes who need dental implants in Peabody, MA, have access to a practice that takes their full medical picture into account – not just their teeth.
Ready to Find Out If Implants Are Right for You?
Managing diabetes and missing teeth at the same time is a lot to carry. The good news is that you don’t have to figure out your options alone. Dr. Brzoza at Coastal Dental Arts takes a thorough, medically informed approach to every implant consultation – which means your diabetes won’t be an afterthought.
Book your consultation on our online site or call the office directly. Come in, ask your questions, and leave with a clear picture of what’s possible for your smile.
People Also Ask
Most oral surgeons and implant dentists aim for an HbA1c below 7.0% before proceeding with implant placement. Some providers will consider patients with levels up to 8.0% if other health indicators are favorable and the patient demonstrates consistent glucose management. Anything above 8.0% typically warrants stabilization before surgery is scheduled.
The type of diabetes matters less than how well it’s controlled. Both type 1 and type 2 patients can be successful implant candidates when blood sugar is stable. Type 1 patients tend to have a longer history of diabetes management and may already have established routines that support good surgical outcomes. The evaluation process is the same regardless of diabetes type.
Often, yes — though it’s determined case by case. Prophylactic antibiotics are commonly prescribed for diabetic implant patients to reduce infection risk during the healing window. Your provider will outline the specific protocol based on your health history, current medications, and the scope of the procedure.
Gingivitis — the early stage of gum disease — is reversible with professional cleaning and improved home care. Advanced periodontitis involves bone loss that can’t be fully reversed, but it can be stabilized and managed. For implant candidacy, the goal is stable, non-active gum disease — not necessarily perfect gum health from the start.